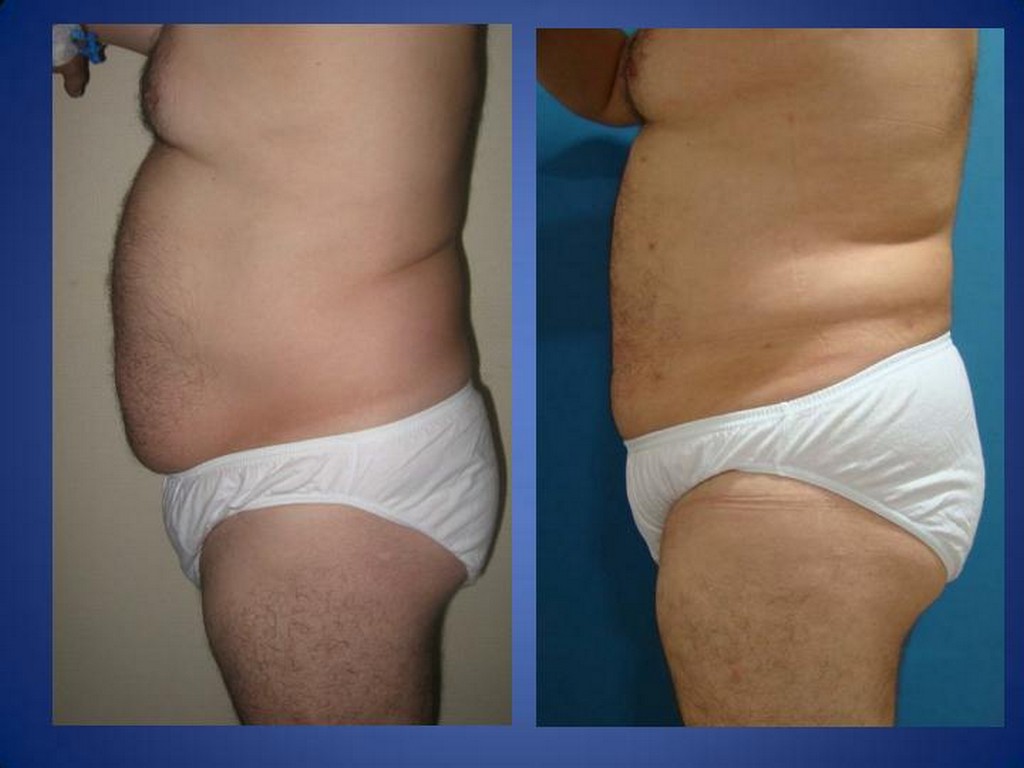
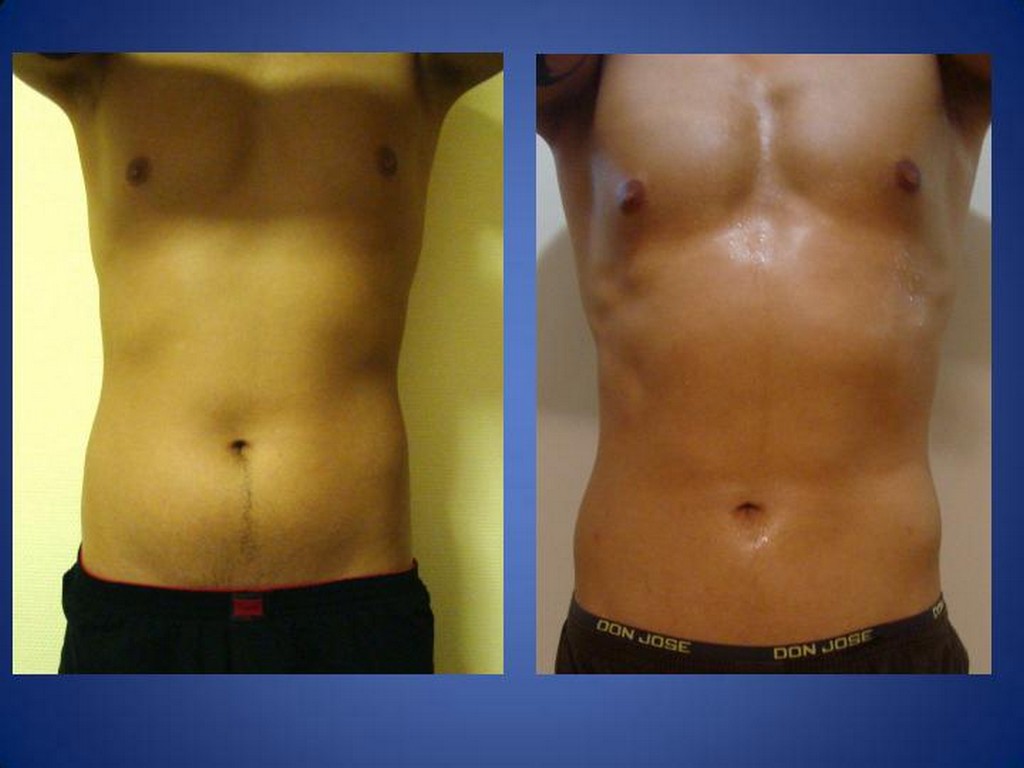
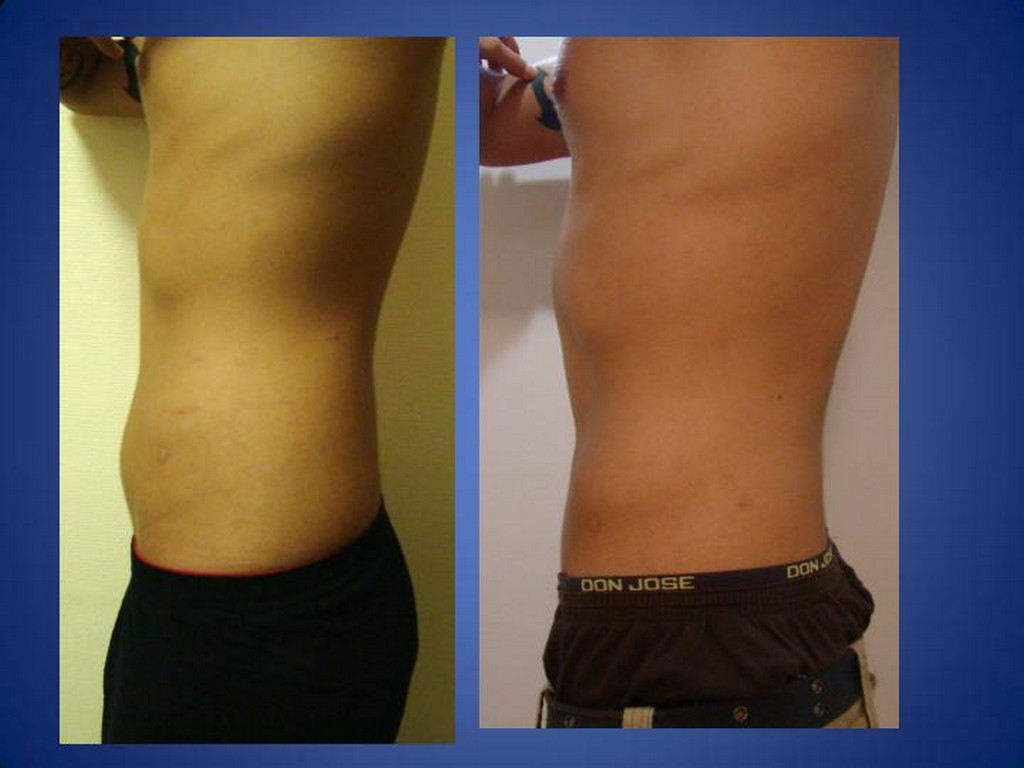
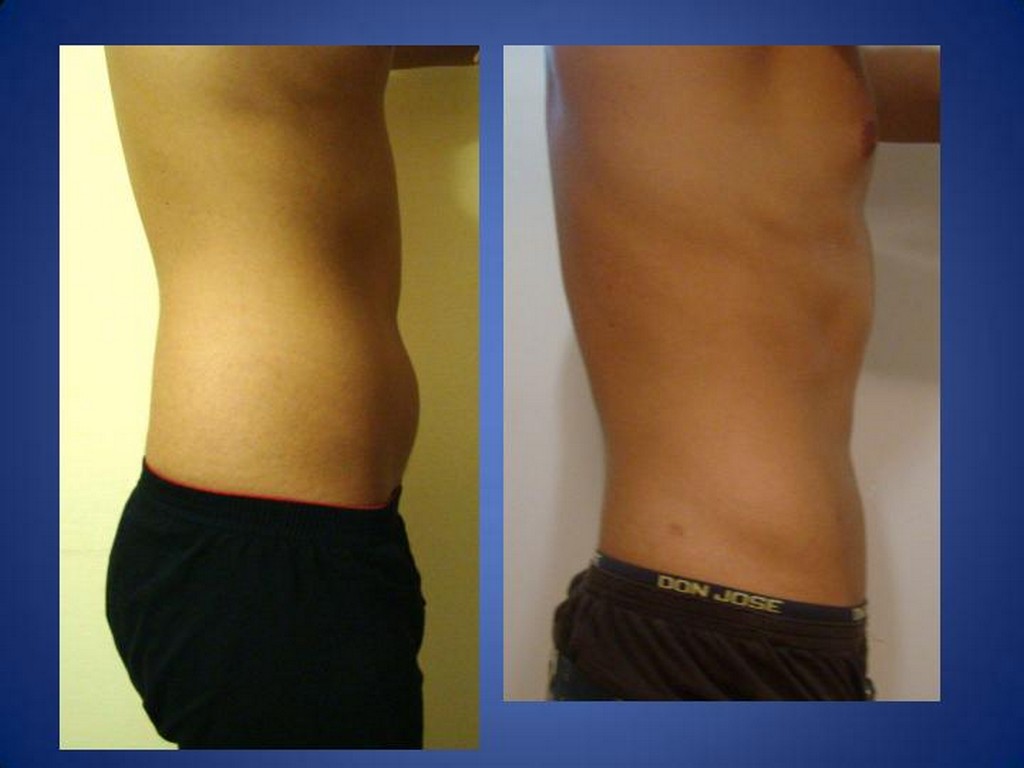
WHAT IS AN ILEAL INTERPOSITION?
Ileal interposition is a metabolic surgery procedure to surgically treat overweight diabetics. The number of type 2 diabetics has increased tremendously in recent decades. Unfortunately, most treatment methods fail to achieve effective success. Surgical procedures for the treatment of type 2 diabetes, on the other hand, have proven to be extremely effective. In this context, metabolic function is the decisive factor in the choice of surgical method.
Ileal interposition surgery is a surgical treatment method that was developed specifically for the treatment of type 2 diabetes and was not intended solely as an obesity surgery. With ileal interposition surgery, it is possible to treat all components of the disease, such as high blood pressure and high cholesterol, with one procedure. The surgery is one of the most effective methods of completely curing type 2 diabetes.
Before surgery, the pancreas is closely examined and its ability to produce insulin is checked. Ileal interposition can only be performed on type 2 diabetics. Before the surgery, patients should pay more attention to their health, as the surgery can only take place if they are in good physical condition. For 1 week before and after ileal interposition surgery, patients should not smoke, drink alcohol, or take blood-thinning medications, such as aspirin.
Who Is Ileal Interposition Suitable For?
A number of examinations and tests are necessary to ensure that a patient is suitable for ileal interposition. A complete blood count, lipid profile, liver function tests, kidney function tests, a pulmonary function test, chest x-rays, an electrocardiogram, and an ultrasound of the entire abdomen may be necessary.
Particularly suitable are slim or normal-weight diabetics who are younger than 65 years old, have had type 2 diabetes for more than 2 years, and have noticed a steady deterioration in their condition because taking medications and making lifestyle changes have not had the success they had hoped for. The procedure is also well suited for patients with a high genetic predisposition and those at risk of complications in other organs.
How Is Ileal Interposition Carried Out?
An eye exam and dental exam provide information about the extent of diabetes-related complications and are used to reduce the likelihood of postoperative infection.
Patients are hospitalized 2-3 days prior to the procedure and are placed on a liquid-only diet.
Like all methods of bariatric and metabolic surgery, ileal interposition is performed without a major abdominal incision (laparoscopic surgery) when possible. In this method, the entire surgery is performed through 1 cm small incisions in the abdomen.
In ileal interposition surgery, the last and the first part of the small intestine are replaced, and the last part is connected to the duodenum. As a result of this procedure, hormones that cause insulin resistance are decreased and hormones that cause sensitivity to insulin are increased.
The procedure is performed under general anesthesia and takes an average of 4 to 5 hours.
Possible Risks
Possible risks include swelling, bleeding and blood clots, internal intestinal hernia, infection, cardiac arrhythmias.
After an Ileal Interposition
Patients must stay in the clinic for 4 to 5 days.
Approximately 6 hours after the procedure, the patient is allowed to consume water; other liquids are not allowed until 2 days after the procedure. Semi-solid food is allowed about 8 days after the procedure.
After about 10 to 15 days, the patient can return to work.
We recommend that patients follow a strict diabetic diet plan, eating smaller meals 3 to 4 hours apart. Slow-digesting carbohydrates (whole grains, fruits and vegetables), plenty of protein and smaller amounts of unsaturated fatty acids from natural sources (walnuts, olive oil and almonds) are an integral part of the new diet.
Sufficient exercise and sport serve to boost metabolism and regulate blood glucose levels. About 2 weeks after the procedure, patients should start exercising slowly and then gradually increase it.
This procedure is a very promising measure for treating patients with type 2 diabetes. Type 1 diabetics can no longer produce insulin because all B cells in their pancreas have been destroyed due to autoimmune reactions or trauma. Type 2 diabetics, on the other hand, do still produce insulin, which is a basic requirement for successful treatment. Indeed, manipulation of the gastrointestinal structure is intended to stimulate the B cells of these patients through physiological stimulation, thereby increasing the natural release of insulin during eating.
Clinical studies demonstrate effective control of blood glucose levels. The success rate is between 80 and even 100 %, which is strongly influenced by the postoperative behavior of the patients.
We would be happy to advise you on the new ileal interposition procedure. For further questions and information about a treatment in Turkey, please contact our Care Team.